Locations
Resource Links


Mental health affects how we think, feel, and live every day; however, it remains one of the most misunderstood and stigmatized aspects of human health. At some point in our lives, nearly all of us will struggle with our mental health, yet many will suffer in silence. With growing social issues surrounding the current political climate, the substance abuse epidemic, and persistent economic inequality, poor mental health continues to rise. It is estimated that “more than one in five U.S. adults live with a mental illness (59.3 million in 2022, 23.1% of the U.S. adult population)” (National Institute of Mental Health, 2024). Figure 1 displays the prevalence of mental health illnesses across the United States, with the majority being young adults and a similar prevalence across all races and ethnicities.
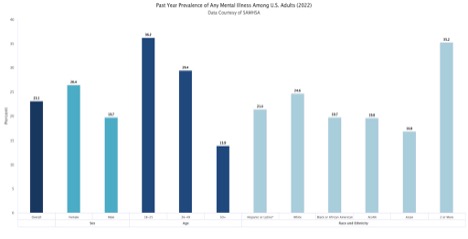
Primary care providers (PCPs) often serve as the first point of contact for patients opening up about mental health concerns. Throughout my family medicine clinical rotations, it was apparent that many PCP offices struggle with time constraints throughout the day. As they attempt to get through medication reconciliation, physical exam, and ordering routine tests in as short as fifteen-minute time slots, mental health can be pushed to the back burner. In a sample of primary care physicians, it was reported, “the average number of patients on a PCP’s [primary care providers] caseload was 3461, and on average PCPs identified 30.3% of their patients as mental health patients” (Faghri, Boisvert, and Faghri, 2010).
Implementing standardized psychiatric assessments such as GAD-7, PHQ-9, and AUDIT-C even prior to the patient entering the exam room can help open up more time throughout the visit while still allowing these questions to take place. In addition, routine check-in questions regarding a patient’s mood, stress level, sleep, and appetite can provide great insight into one’s current mental health state and help guide further conversation if needed. As displayed in Figure 2, all PCPs play a role in psychiatric care in one way or another, with the majority having familiarity with prescribing antidepressants and anxiolytics.
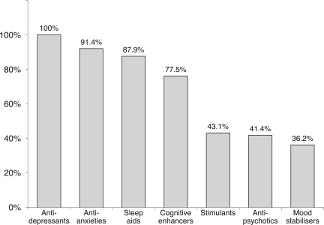
In addition, while volunteering as a Crisis Text Line Counselor, I was able to see firsthand how many individuals throughout the country at any given minute are dealing with mental health crises and looking for someone just to listen to their story. We were trained to ask difficult questions regarding suicidal ideations and how to implement a safety plan if needed, and I think that’s something all physicians should have a comfort level in, regardless of the specialty. Simply showing compassion and emphasizing the bravery of the individual for reaching out helps normalize what the individual is going through. Furthermore, a positive experience with a health care professional could encourage them to continue seeking support and improve overall adherence.
How we can improve: First, having awareness of resources and referral contacts throughout the community, including nonprofit organizations that offer mental health services, will serve as a vital skill going forward. This will help grow awareness of resources such as telehealth services, which could increase access to rural neighborhoods. As portrayed by Figure 3, the majority of the country significantly lacks the resources necessary to cover mental health needs.
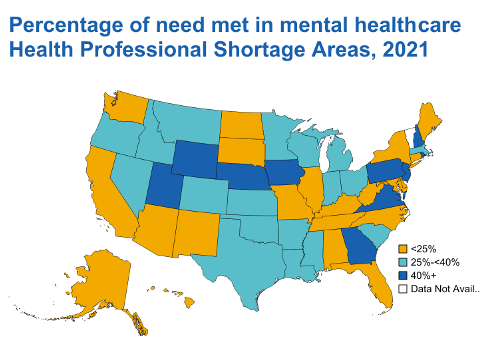
In addition, providing patients with tools for self-care and coping strategies, including regular exercise, maintaining an adequate sleep schedule, and breathing techniques, will allow patients to incorporate self-care in their daily schedules and hopefully reduce crises. Such simple interventions could also be provided in a handout during or after primary care visits to reduce the necessary time throughout the exam. Finally, incorporating mental health training modules or simulated psychiatric patient encounters into continuing medical education for physicians would allow for early identification of mental health disorders and adequate intervention. Overall, creating a safe environment for open discussion with patients will help prevent individuals from being undertreated or underrecognized.
 Katelyn is a third-year osteopathic medical student attending Marian University Wood College of Osteopathic Medicine. She is passionate about improving health and social disparities, patient advocacy, and reproductive mental health, and is currently considering a field in psychiatry. In her free time, she loves to be outdoors, trying new restaurants, and spending time with loved ones. Feel free to email her if you have any questions!
Katelyn is a third-year osteopathic medical student attending Marian University Wood College of Osteopathic Medicine. She is passionate about improving health and social disparities, patient advocacy, and reproductive mental health, and is currently considering a field in psychiatry. In her free time, she loves to be outdoors, trying new restaurants, and spending time with loved ones. Feel free to email her if you have any questions!
Abed Faghri, N. M., Boisvert, C. M., & Faghri, S. (2010). Understanding the expanding role of primary care physicians (PCPs) to primary psychiatric care physicians (PPCPs): enhancing the assessment and treatment of psychiatric conditions. Mental health in family medicine, 7(1), 17–25.
Amutio-Kareaga, A., García-Campayo, J., Delgado, L. C., Hermosilla, D., & Martínez-Taboada, C. (2017). Improving Communication between Physicians and Their Patients through Mindfulness and Compassion-Based Strategies: A Narrative Review. Journal of clinical medicine, 6(3), 33. https://doi.org/10.3390/jcm6030033
Modi H, Orgera K, Grover A. Exploring Barriers to Mental Health Care in the U.S.Washington, DC: AAMC; 2022. https://doi.org/10.15766/rai_a3ewcf9p
National Institute of Mental Health. (2024, September). Mental Illness. National Institute of Mental Health. https://www.nimh.nih.gov/health/statistics/mental-illness
Discover the voices of Marian University's health professions students through "Franc Notes", a vibrant, student-led blog that embodies our Franciscan commitment to community, reflection, and compassionate service. Inspired by the rhythm of "SOAP notes," it features weekly insights—from "DO Diaries" interviews with physicians to summer reflections and program spotlights—fostering collaboration across disciplines."