Doctor of Osteopathic Medicine Degree
Marian University’s Doctor of Osteopathic Medicine (DO) program has had proven success in preparing students for their residency and future careers. Our College of Osteopathic Medicine is an accredited institution conveniently located in Indianapolis. Based on our Franciscan values, our DO program emphasizes education based on improving the health of mind, body, and spirit.
Admission requirements to the DO Program
DO Degree Curriculum
The Marian University College of Osteopathic Medicine (MU-COM) features state-of-the-art classrooms, laboratories, study areas, and a simulation center. The curriculum in the DO program was designed to facilitate progressive achievement of the seven core competencies
enunciated by the National Board of Osteopathic Medical Examiners
(NBOME), and to address key recommendations from the Carnegie report,
Educating Physicians: A Call for Reform of Medical School and Residency, which is an important review of the methods and practices of medical education over the last 100 years. This ensures that students are receiving up-to-date training on crucial
aspects of osteopathy.
Our integrated, patient-centered curriculum has been designed to prepare the next generation of physicians to have successful careers in all areas of medicine. DO courses have a clinical basis, giving you hands-on experience that will carry over to professionally working with patients. A variety of teaching methods, including lectures, laboratories, case-based seminars, podcasts, team-based learning, and early clinical experiences, give you a unique opportunity to master the core aspects of osteopathic medicine.
Matriculating students are referred to as Osteopathic Medical Students (OMS-I, II, III, and IV). Hospitals and other healthcare employers are seeking physicians who have the ability to work in an ever-changing healthcare environment.
New Professional Identity Formation Series
 Professional Identity Formation (or PIF) is a longitudinal curriculum that is delivered across all four years of the medical school experience at Marian University College of Osteopathic Medicine.
Professional Identity Formation (or PIF) is a longitudinal curriculum that is delivered across all four years of the medical school experience at Marian University College of Osteopathic Medicine.OMS-I and OMS-II: Preclinical Curriculum
MU-COM offers a uniquely integrated and team-based approach to the medical training curriculum by integrating didactic and clinical competencies, offering inter-professional education with nursing students, including a clinical basis to biomedical science courses, and providing you with clinical experiences in your first and second years of medical school.
 Courses are taught by our experienced faculty.
Biomedical and clinical faculty will help you obtain the knowledge needed to successfully treat the root cause of a disease, but also show the compassion and patient-centered approaches central to osteopathic medicine. They will also help you attain
the foundation to be highly successful during your clinical rotations in years three and four.
Courses are taught by our experienced faculty.
Biomedical and clinical faculty will help you obtain the knowledge needed to successfully treat the root cause of a disease, but also show the compassion and patient-centered approaches central to osteopathic medicine. They will also help you attain
the foundation to be highly successful during your clinical rotations in years three and four.
To help achieve this understanding, faculty will help you understand the systems and structures of the human body in our state-of-the-art anatomy lab, better understand how structure and function work together; develop your hands into treatment instruments by utilizing our osteopathic manipulative medicine (OMM) lab as well as teach you examination procedures using our simulation and examination rooms.


OMS-III and OMS-IV: Clinical Core Curriculum
During the third year, students transition from classroom-based learning to clinical training, where they spend more time in direct patient care settings.
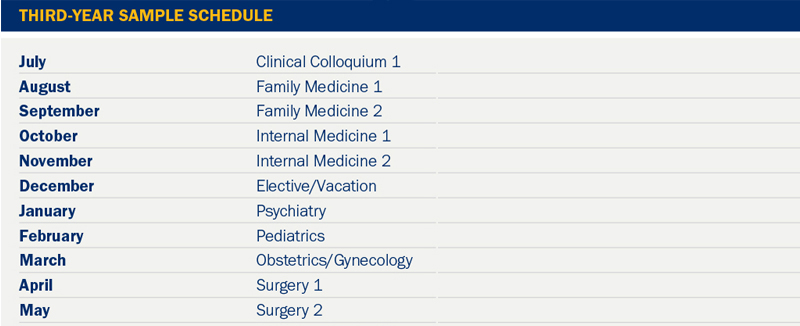
The third-year curriculum is made up of ten months of clinical rotations, with nine months of core rotations and one month of an elective rotation. Each student completes two one-month rotations in Family medicine, Surgery, and Internal Medicine; and one one-month rotation in Psychiatry, Pediatrics, and Obstetrics/Gynecology, and an elective month in a clinical specialty of their choice.
The third and fourth years follow an apprenticeship model, where students work closely with physicians or preceptors in various medical specialties. This immersive experience allows students to apply their knowledge and skills in real-world healthcare settings under preceptor supervision. Students also dedicate time to studying for exams, such as end-of-rotation Comprehensive Osteopathic Medical Achievement Tests (COMATs) and Comprehensive Osteopathic Medical Licensing Examination (COMLEX) Level 2-CE.
During the third year, students also start exploring and finalizing their desired medical specialties. This involves working with faculty or physicians to obtain letters of recommendation and preparing residency applications.
The fourth-year curriculum is made up of ten months of clinical rotations that include a sub-internship, selective, and elective rotations which align with students' career goals and desired specialty.

College of Osteopathic Medicine (MU-COM) Compliance
In compliance with the U.S. Department of Education regulation 34 CFR 668.43 (a) (5) (v) MU-COM, accredited by the Commission on Osteopathic College Accreditation (COCA), acknowledges:
- The curriculum of MU-COM meets the educational requirements for a Doctor of Osteopathic Medicine (DO) degree, recognized by all states as the required DO degree for licensure.
Any student planning to relocate to another state after completion of the program can seek guidance from Regina Obergfell, Assistant Registrar for Graduate and Professional Health Science Programs, for documentation of the DO degree or the Sr Advisor to the Sr Vice President of Health Professions, Elizabeth Petsche, JD, to determine whether the curriculum meets the educational requirements for licensure/certification in that state.
Marian University’s Doctor of Osteopathic Medicine degree features a proven track record of student success with state-of-the-art facilities. Interested in learning more?
Guiding Principles and Practice
MU-COM is dedicated to the promotion of a learning environment that is conducive to the ongoing development of professional behaviors in students, faculty, staff, and administration and is one in which all individuals exhibit mutual respect. This includes facilitating the exposure of learners to aspects of quality and safety, cultural competence, and interprofessional collaborative practice.
Our learning environment is consistent with the Catholic Mission of Marian University and based upon the four Franciscan Values given to us by the Sisters of Saint Francis: Dignity of the Individual, Reconciliation, Responsible Stewardship, and Peace and Justice. In addition, the curriculum of MU-COM is based upon the articulated expectations and requirements of professional organizations, national licensure boards, and accrediting bodies. The faculty of MU-COM is committed to meeting these expectations and requirements, while striving to not promote or endorse any personal view, opinion, or belief. Our guiding principles and practice can be found here.
© 2021 Marian University
Notice of Nondiscrimination
Marian University does not discriminate on the basis of race, ethnicity, color, sex, gender, gender identity, sexual orientation, religion, creed, national origin, age or disabilities in the selection
of administrative personnel, faculty and staff, and students.
*Placement rates are gathered from data collected from graduates within six months of graduation.
Students may make a complaint to the Indiana Commission of Higher Education.
Marian University is sponsored by the Sisters of St. Francis, Oldenburg, Indiana.
Submit a Marketing Request
Website built with
